Introduction
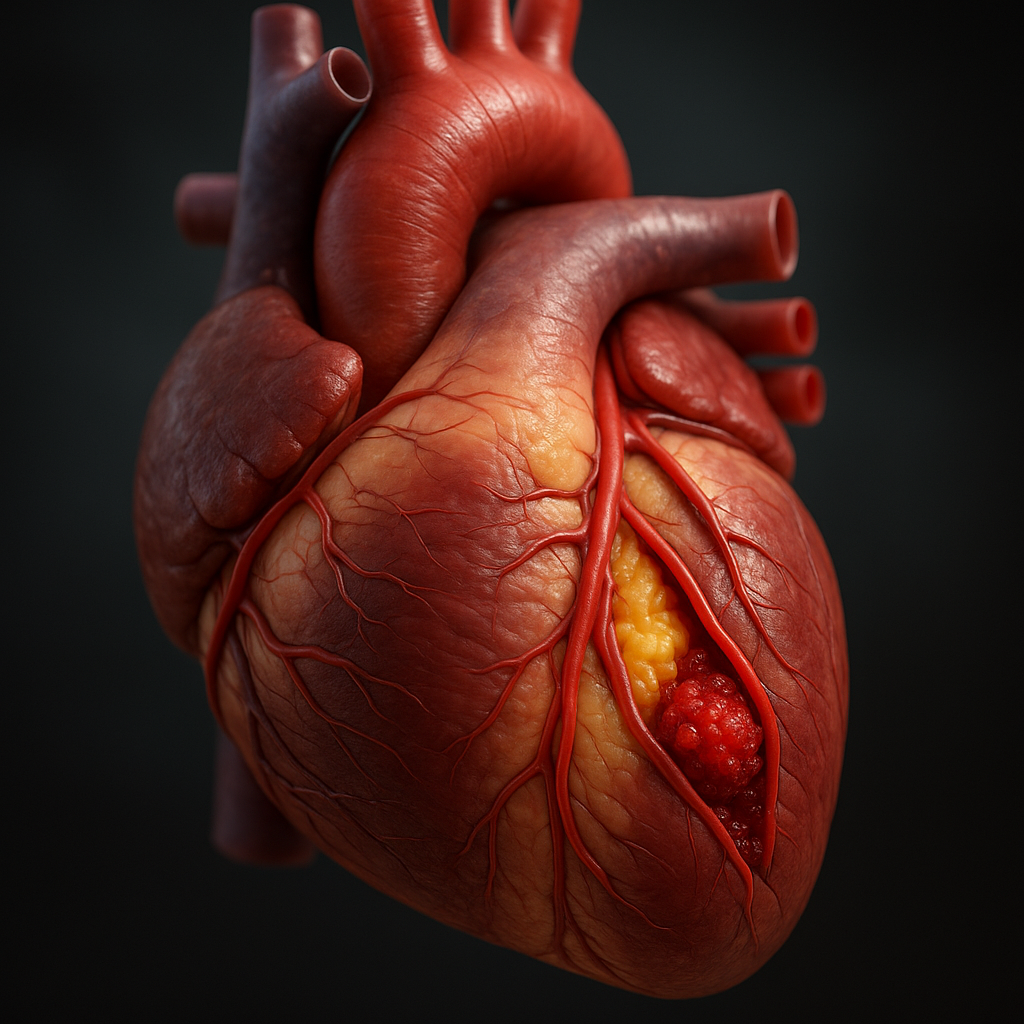
A heart attack (Myocardial Infarction) is a critical cardiovascular emergency that can lead to death or permanent damage within minutes. Due to the fast-paced lifestyle and deteriorating health habits of modern times, it has become more common than ever. As a specialist, my goal with this article is to help you understand how to recognize a heart attack, identify alarming symptoms, and make lifestyle changes that can keep your heart healthy.
1. What is a Heart Attack? (Definition & Mechanism)
A heart attack occurs when the blood flow to a part of the heart muscle is suddenly blocked. Coronary arteries are the small vessels that supply oxygen and nutrients to the heart. When these arteries become blocked—primarily due to cholesterol deposits and plaque buildup—oxygen supply is cut off to that part of the heart. Within minutes, muscle tissue begins to die, leading to lasting damage that can affect overall heart function for life.
2. Causes of Heart Attack (Etiology)
2.1 Coronary Artery Atherosclerosis
High levels of cholesterol, triglycerides, and fats in the blood can gradually accumulate on artery walls, forming plaque. Over time, these plaques may rupture, causing clot formation inside the arteries, blocking blood flow.
2.2 High Blood Pressure (Hypertension)
Uncontrolled blood pressure stiffens and damages the artery walls, increasing the risk of blockage and hypertensive heart disease.
2.3 Smoking and Alcohol
Smoking reduces arterial elasticity, raises blood pressure, and encourages clot formation. Alcohol can induce oxidative stress in heart cells, causing further arterial damage.
2.4 Diabetes & Metabolic Syndrome
Elevated blood glucose levels weaken artery walls and increase the likelihood of plaque formation and heart attacks.
2.5 Mental Stress and Lifestyle Imbalance
Chronic stress raises cortisol and adrenaline levels, placing added strain on the heart and increasing blood pressure.
2.6 Genetic Predisposition
If close family members experienced heart attacks at a young age, your personal risk may be significantly higher.

3. Symptoms (Clinical Presentation) https://amzn.to/3GtPzDh
Mnemonic: “OLD CLOTS”
- O – Over-chest pressure (tightness or heaviness in the chest)
- L – Left arm or shoulder pain
- D – Diaphoresis (cold sweating)
- C – Chest discomfort (burning, heaviness, or pressure)
- L – Loss of consciousness or extreme weakness
- O – Oxygen shortage (shortness of breath)
- T – Tachycardia or palpitations
- S – Sick feeling (nausea, vomiting)
Symptoms in Women & Elderly Patients
Women may not experience classic chest pain. Instead, they may present with nausea, unusual fatigue, breathlessness, or anxiety. Hence, such symptoms should not be ignored.
4. Immediate Actions (First Aid Protocol)
- Call Emergency Services Immediately
- Keep the patient seated or in a semi-reclined position
- Administer Aspirin (300 mg) if readily available
- Provide Nitroglycerin only if it was previously prescribed
- At the hospital: Perform ECG, Troponin tests, and other diagnostics promptly
The first 1–2 hours are known as the “Golden Hour”, where timely treatment can protect heart function and save lives.
5. Diagnosis Methods
5.1 ECG (Electrocardiogram)
Useful for identifying ST-segment elevation and categorizing the type of MI.
5.2 Troponin & CK-MB Blood Tests
Elevated cardiac enzyme levels (especially Troponin) strongly indicate recent heart damage.
5.3 Imaging Techniques
- Echocardiography: Evaluates wall motion and muscle function.
- Angiography: Provides real-time visuals of blocked arteries and guides revascularization plans.
6. Treatment Options
6.1 Initial Medications
- Aspirin & P2Y12 Inhibitors (e.g., Clopidogrel) – to inhibit platelet aggregation
- Beta-Blockers – to reduce heart workload
- ACE Inhibitors / ARBs – to control blood pressure and cardiac strain
- Statins – to manage cholesterol
6.2 Revascularization Procedures
- Primary PCI (Percutaneous Coronary Intervention): Placement of a stent in the blocked artery
- Thrombolysis: Administering clot-dissolving drugs to restore blood flow
6.3 Intensive Care & Rehabilitation
- ICU Monitoring: To manage complications like heart failure or arrhythmias
- Cardiac Rehab: Includes exercise training and lifestyle counseling for long-term heart health
7. Post-Attack Recovery & Lifestyle Modification https://amzn.to/3GtPzDh
7.1 Diet Changes
- Increase intake of vegetables, fruits, and whole grains
- Low-fat dairy
- Healthy fats like olive oil, nuts, and fatty fish (salmon)
7.2 Regular Exercise
- 4–5 days/week of 30–50 minutes of moderate activity (e.g., walking, swimming)
- Supervised strength training if needed
7.3 Weight & Diabetes Management
- Maintain BMI between 23–25
- Keep HbA1c < 7%
7.4 Blood Pressure & Cholesterol Control
- Blood pressure <130/80 mmHg
- LDL cholesterol <70 mg/dL
7.5 Avoid Tobacco and Limit Alcohol
- Quit smoking completely
- Alcohol: Maximum 10–12 grams per day
7.6 Stress Management
- Meditation, yoga, breathing exercises
- Maintain healthy relationships and social interaction
7.7 Routine Check-ups
- Every 3–6 months: ECG, Echo, Lipid Profile
- Adhere strictly to prescribed medications

8. Complete Prevention Strategy (Zero-Risk Lifestyle)
If you adopt healthy habits early—such as quitting smoking, eating right, regular physical activity, and managing stress—you can reduce your risk of heart attack by 50–70%. With discipline and awareness, heart attacks are largely preventable.
9. FAQs (Frequently Asked Questions)
Q1: Are “Stroke” and “Heart Attack” the same?
A: No. Stroke affects the brain due to interrupted blood flow, while a heart attack involves the heart. However, both are caused by blood vessel blockages.
Q2: Will heart patients need lifelong medication?
A: Not always. With disciplined lifestyle changes, medications can sometimes be reduced or stopped—under medical supervision only.
Q3: How long is hospital recovery time?
A: Basic testing takes 4–6 hours. After PCI, ICU observation is typically 48 hours. Discharge is possible within 1–2 weeks in stable cases.
Conclusion
A heart attack is rarely a sudden event—it often develops gradually over time. Careful attention to diet, exercise, medications, and mental health can keep you safe. As a medical professional, I emphasize: a regulated lifestyle is your strongest defense.
🔑 Key Takeaways:
- Be proactive and aware of early warning signs
- Seek timely diagnosis and treatment
- Commit to long-term lifestyle transformation
Omega-3 Fatty Acid Supplements
Proven heart benefits
Reduces blood triglycerides

- Coenzyme Q10 (CoQ10) Supplements
Supports heart function
Very important for those taking statin drugs

- Blood Pressure Monitor (Digital BP Machine)
Use it to measure blood pressure at home to stay alert

5. Heart Rate Monitoring Smartwatches
Very useful for monitoring your heart rate while exercising, running, or doing any work.
Disclosure: This article may contain affiliate links. If you purchase through these links, I may earn a small commission at no extra cost to you. Thank you for supporting this site.